
Health

Obamacare: Promises Made, Promises Broken
When Barack Obama ran for president in 2008, health care was a major issue. Although many on the left were advocating single-payer, national health insurance, Obama pledged private health insurance reform instead.

April 2022 Health Care News
In this post you will find the latest topics from The Health Care News publication.
Covid: Could We Have Saved More Lives?
According to a Goodman Institute study by David Henderson and Charles Hooper, studies suggest that there are at least 11 drugs that can substantially reduce mortality in patients who contract Covid-19. These drugs are widely used, safe, and convenient. Because they are generic, most of them cost $1. A few of them cost $5.

Did the Government Make us Fat?
Beginning around 1980, the federal government and public health agencies began demonizing meat and saturated fat as the major cause of obesity, diabetes, and cardiovascular disease in the U.S. and around the world. They promoted a low-fat diet with increased consumption of carbohydrates instead. Obesity in the US has been steadily increasing ever since.
Sadly, these top-down public health campaigns served up a perfect nutritional storm for higher levels of obesity, diabetes, high blood pressure, and cardiovascular disease. And this was done while mounting, high-quality, peer-reviewed nutritional research suggested the basis for their advice was completely wrong.

New Partnership: Health Care News
Because of budget shortfalls, the Heartland Institute suspended publication of Health Care News in March. Fortunately, the Goodman Institute for Public Policy has agreed to partner with Heartland to ensure the newspaper’s survival going forward.

Kotlikoff: Beating COVID-19 with Math
A strategy for extinguishing the novel coronavirus has been outlined by Cornell University’s Operations Research Professor Peter Frazier and colleagues. They developed a group testing protocol that could release 96 percent of the U.S. population back to society within four weeks, with this percentage rising even higher thereafter. Frazier envisions initially testing 62 households at a time, and assumes, to be conservative, a very high (30 percent false negative) test rate that would require some degree of redundancy to work efficiently. All told, though, the job could be done for the entire United States with only 6 million tests per week. That’s a large number, but just three to four times the test rate we’ve already reached.
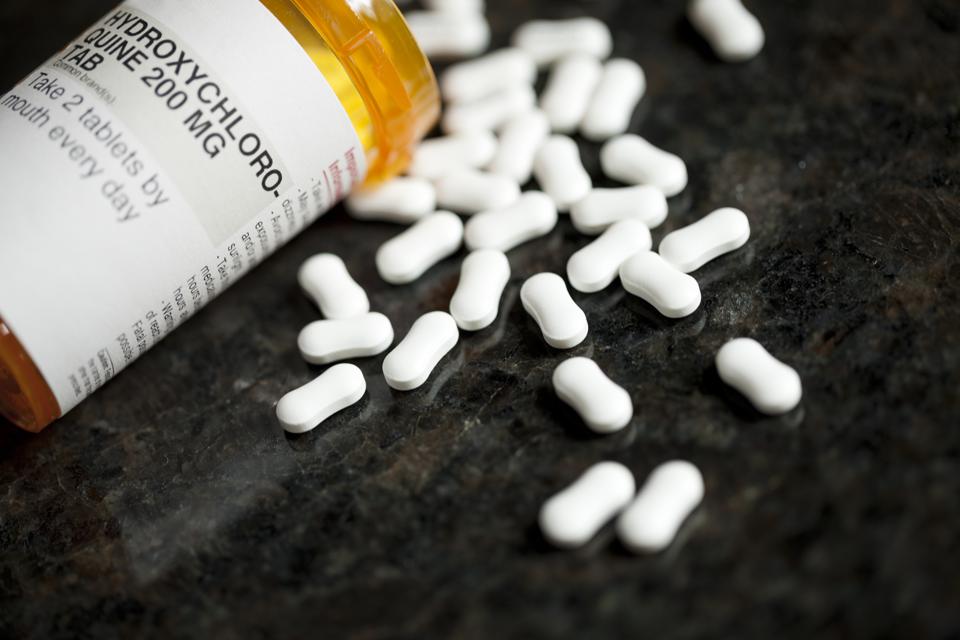
Study: Liberate Prescription Drugs
The mainstream media had a field day condemning Donald Trump for promoting off-label uses of prescription drugs to treat the coronavirus. So what do you expect to happen when a drug is “proven”? Did you know that “approved” drugs work only half the time? What about “unproven” drugs? Did you know that as many as one in five drugs in use in the United States has been prescribed for an off-label purpose? Roughly one-half of all cancer patients are relying on off-label prescriptions. Much of what doctors know they learn by trial and error – outside of FDA tests.

How COVID-19 Is Changing The Debate Over Health Reform
A revolution is occurring in the way medical care is being delivered in the United States. It is happening almost overnight. People have stopped going to hospital emergency rooms. They have stopped going to doctors’ offices. Most of the nation is self-isolating. Doctors and patients are no exception. They are communicating by means of phone, email, Skype, Zoom and other devices. Last December, Zoom was the host of 10 million video conferences a day. Last week, the company was hosting 200 million a day. Many of those were patient/doctor communications.
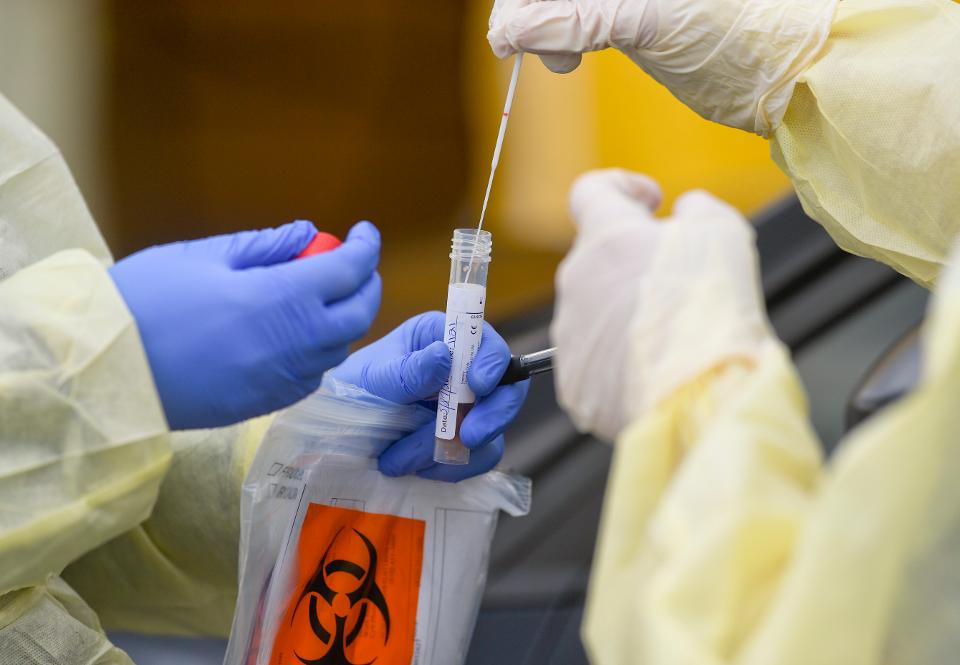
Kotlikoff: we need group testing, every day
With group testing, you take samples, say, from 20 people and test them all at once. If the result is negative, those 20 are free to go to work. If the test is positive, you divide the group into two and test 10 at a time. Using this method, you greatly reduce the number of tests needed to separate those who have the virus from those who do not. And we should do this every day.
Coronavirus and Health Reform
Critics of President Trump’s response to the coronavirus crisis characterize it as knee-jerk, spur-of-the-moment, and grasping at any straw within reach. In fact, many of the executive actions we have seen in the past few days reflect a new approach to health policy that has been underway almost since the day Donald Trump was sworn into office.
These include the ability to be diagnosed and treated without ever leaving your own home; the ability to talk to doctors 24/7 by means of phone, email and Skype; and the ability of the chronically ill to have access to free diagnoses and treatments without losing their access to Health Savings Accounts.