
Devon Herrick’s Commentaries

The Perils of Trying to Become a Doctor
This week the National Resident Matching Program (Match) will inform between 45,000 to 50,000 medical graduates whether they have a career in medicine or should try for Plan B. Some of those who failed to match (about 20 percent) will spend the rest of their lives trying to pay down $300,000 in medical school debt without an income capable of servicing that debt.
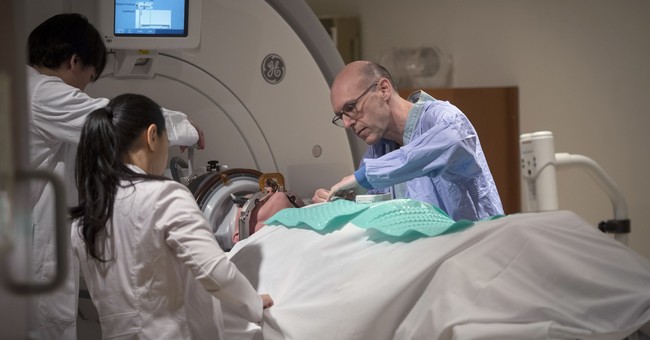
How a Questionable Drug Turned into a Goldmine at Taxpayers’ Expense
On June 7th the U.S. Food and Drug Administration approved a new drug to treat early-stage Alzheimer’s disease. Is this good news for patients suffering with Alzheimer’s disease? Probably not and certainly not for taxpayers. The clinical trial data found little evidence the drug works. One Phase 3 clinical trial showed a slight slowing in cognitive decline, while the second clinical trial failed to show any improvement.
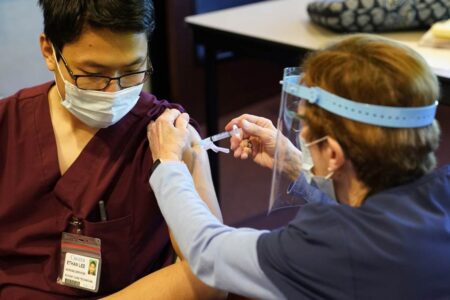
What’s Behind the Vaccine Slowdown?
What’s behind the slowdown in vaccinations? The consensus among experts is those not yet vaccinated either 1) don’t want the vaccine 2) harbor some doubts about vaccine safety or efficacy, or 3) simply lack the motivation to find vaccine providers and make an appointment. Vaccine hesitancy accounts for about one-third of adults. For example, the Kaiser Family Foundation ran a survey in April that found 15 percent of respondents who had not received the vaccine plan to “wait and see.” Another 6 percent will get vaccinated “only if required,” and 13 percent refuse to get the vaccine.
Correcting Misconceptions of Health Care Reform
One reader posed the question, how does the tax break for employee health insurance harm our health care system? Short answer: over time the practice reduced competition, which weakened cost-control and resulted in health care inflation three times that of consumer inflation. Consider this: once covered by generous health plans, workers cared less about what medical care cost because their health plans paid most of the tab. Employers didn’t care what things cost because they were passing on the costs to workers (indirectly) in lieu of higher cash wages. Third party administrators (TPAs), who manage the benefits for employers, didn’t much care what things cost because they were passing on the costs to employers with a mark-up. The more money spent, the more TPAs earn.

Health Reform: There Is Something for Everyone to Love… and Hate
Why is it controversial to expand the physician supply, creating more competition? Doctors oppose it, just like they oppose expanding the scope of practice for nurse practitioners. Doctors don’t want me to be able to see a nurse practitioner or physician assistant for a wart on my toe unless that NP/PA works for them.
How did doctors get so powerful? In the first half of the 20th Century, the American Medical Association (AMA) waged a largely successful battle to close medical schools that trained competing physicians. …. More than half of American and Canadian medical schools were closed…. Thus, the job of a physician was yanked out of reach of all but the smartest, most disciplined, wealthy elites.
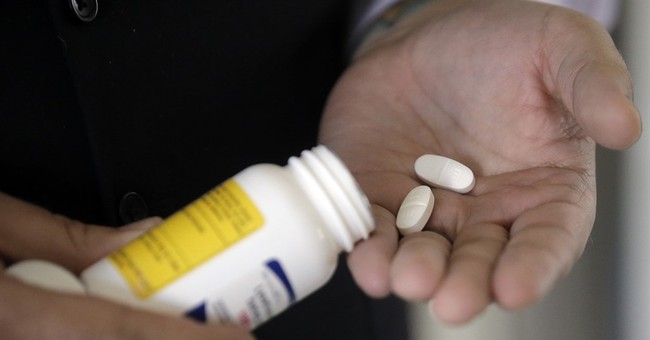
The 60 Percent Solution to Reforming Healthcare
Can we transform the entire health care system by empowering the roughly 60 percent of patients who are in private health plans? That’s the premise of a new book I just read by Todd Furniss (@TFurniss on Twitter). The author ofThe 60% Solution: Rethinking Healthcare, believes there are five major reforms necessary to empower patients and help them get better care at better prices. These include: (1) change governance, (2) modify health savings accounts (HSAs), (3) clear prices, (4) standardize accounting and information technology in the medical industry and (5) emphasize primary care.
Herrick: OBAMACARE RATIONS CARE FOR THE SICK AND OVERCHARGES THE HEALTHY
The health care reform debate that lead to Obamacare was initially about covering the uninsured, but in order to gain the support of ordinary people who already had coverage, proponents had to figure out a way to sway public opinion.
Herrick: States Should Ban These Lab Scams
There is a new health care scam spreading across rural America that could cost you plenty. Large commercial labs like Quest Diagnostics and LabCorp do not have locations in every small town. As a result, many rural hospitals perform lab work for both their inpatients and outpatients in the local community.
Herrick: Future Pandemics Require Better Access to Primary Care
When Americans become ill or have a health complaint, they often schedule an appointment with a primary care provider (PCP). PCPs are often the first line of defense in the battle against the onset of seasonal outbreaks of colds, flu or more serious problems like COVID-19.
Herrick: Could Free-Market Medicine Respond Better to Pandemics?
Many people have come to believe that the only way to protect Americans against future pandemics is to turn over control of our health care system to the government. The folly of this view was apparent when the U.S. Centers for Disease Control & Prevention (CDC) utterly failed as the monopoly supplier of COVID-19 diagnostic testing kits. When the first cases appeared, about half of the test kits failed and replacements were slow in coming.